About VENCLEXTA
WHAT IS VENCLEXTA AND HOW DOES IT WORK?
About VENCLEXTA
VENCLEXTA is prescription medicine in tablet form that is used to treat chronic lymphocytic leukaemia (CLL) and small lymphocytic lymphoma (SLL).
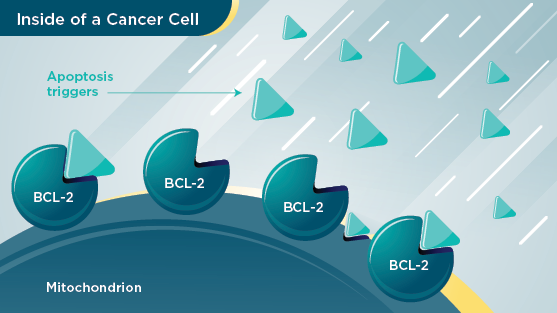
VENCLEXTA contains the active ingredient venetoclax. It works by blocking a protein in the body called “BCL-2” that helps cancer cells survive. It is therefore known as a “BCL-2 inhibitor”.
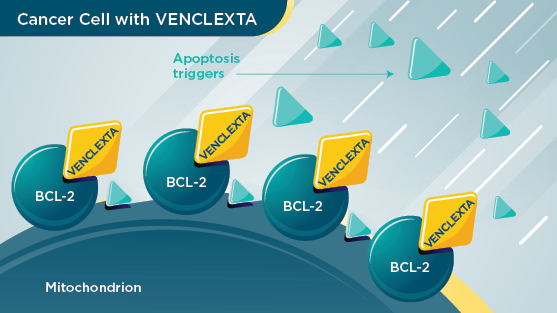
VENCLEXTA sticks to the BCL-2 and blocks it. Without the help of the BCL-2 protein, the cancer cells die.
HOW DOES RITUXIMAB WORK?
About Rituximab
Rituximab works in a different way to VENCLEXTA. It works by binding to an antigen (CD20) on the surface of certain white blood cells known as B lymphocytes. It is the abnormally growing B lymphocytes that are responsible for certain types of lymphoma and leukaemia. During the process of binding to the antigen, the abnormal growth of the B lymphocytes is stopped.
For more information about rituximab, please refer to the Consumer Medicine Information or speak with your doctor or pharmacist.
WHY VENCLEXTA?
VENCLEXTA is designed to offer you:
1. A fixed treatment period
VENCLEXTA is designed to be completed in a set amount of time (~24 months, when combined with rituximab for previously treated CLL/SLL).
2. Limited exposure
Because VENCLEXTA can be taken for a set amount of time, VENCLEXTA exposure is limited.
3. A treatment that is chemo-free
VENCLEXTA is an oral-based, chemo-free treatment for CLL. It will be prescribed with rituximab, which is an antibody given by infusion.
VENCLEXTA in combination with rituximab is fully funded for relapsed CLL. Special authority criteria apply. Normal prescription charges and doctor’s fees apply.
NZ-VEN-200003. TAPS BG5144. June 2025.
For more information about AbbVie, the maker of VENCLEXTA, visit www.abbvie.co.nz
For medical information enquiries regarding VENCLEXTA please contact [email protected]
The content on this site is intended solely for New Zealand residents. The information is intended for informational purposes only and should not be used to replace a discussion with a healthcare professional. All decisions made regarding patient care must be handled by a healthcare professional and be made based on the unique needs of each patient. This website has been developed and is funded by AbbVie Limited, Wellington. The person shown is from stock photography (model) and is not an actual patient.
VENCLEXTA in combination with obinutuzumab or ibrutinib is fully funded for untreated chronic lymphocytic leukaemia (CLL). VENCLEXTA in combination with rituximab is fully funded for relapsed/refractory CLL. VENCLEXTA in combination with azacitidine or low dose cytarabine is fully funded for acute myeloid leukaemia (AML). Special Authority criteria apply. Refer to the VENCLEXTA PHARMAC Special Authority criteria.
IMPORTANT INFORMATION ABOUT VENCLEXTA®
VENCLEXTA® is a prescription medicine containing venetoclax. Venclexta is available as film-coated tablets of various strength (10 mg, 50 mg, 100 mg venetoclax). It is used to treat adults with chronic lymphocytic leukaemia (CLL) or small lymphocytic lymphoma (SLL) or acute myeloid leukemia (AML). Venclexta is taken alone or in combination with other medicines. Your doctor will let you know which combination medicines, how to take them, and how long to take them. Typically, you will start treatment with Venclexta at a low dose. If you are taking Venclexta for CLL or SLL, your doctor will gradually increase your dose over 5 weeks up to the full dose. If you are taking Venclexta for AML, your doctor will gradually increase your dose up to the full dose over 3, or 4 days, depending on the combination medicine used. Use strictly as directed by your doctor. Venclexta has risks and benefits. You must not take it if you are allergic to venetoclax or to any of the inactive ingredients. For CLL or SLL, do not take Venclexta if you are taking any of the following medicines: medicines used to treat or prevent fungal infections, including ketoconazole, posaconazole, voriconazole, itraconazole; clarithromycin (an antibiotic); or ritonavir (a medicine used to treat HIV and hepatitis C). Do not drink grapefruit juice, or eat grapefruit, starfruit or Seville oranges or marmalades. Do not give Venclexta to children and adolescents under 18 years of age. Do not take Venclexta if you are pregnant or plan to become pregnant, or if you are breastfeeding or plan to breastfeed. If you are a woman of child-bearing age, you must use a highly effective form of contraception during treatment with Venclexta and for at least 30 days after your last dose. Tell your doctor, nurse, or pharmacist if you have any kidney or liver problems; if you think you may have an infection; or if you recently received or are scheduled for any vaccinations. Do not stop using Venclexta or change the dose without checking with your doctor. Venclexta can cause tumour lysis syndrome (TLS), which is caused by the fast breakdown of cancer cells. TLS is a very serious side effect that can be fatal. TLS is most likely to occur when you are first starting treatment. To help prevent TLS, it is important to stay hydrated and drink water every day when taking Venclexta. Particularly, starting two days before and on the day of your first dose of Venclexta and every time the dose is increased, drink 6 to 8 glasses (approximately 1.5-2 L total) of water each day. Let your healthcare provider know immediately if you experience: fever or chills; feeling sick or vomiting; being short of breath; feeling unusually tired; changes in your heart rate (slow, fast or irregular); your urine looks dark or cloudy; feeling confused; convulsions or fits; or pain in the muscles or joints while on treatment with Venclexta. Ensure you follow all your doctor’s instructions carefully and keep all your appointments, including those for blood tests. You may experience a low number of neutrophils, a type of white blood cells – this can be severe and need treatment. Your doctor will check your blood counts during treatment with Venclexta. You may experience infections during treatment with Venclexta. Some infections can be very serious or even fatal. Your doctor will closely monitor and treat you right away if you have fever or any signs of infection during treatment with Venclexta. Tell your doctor immediately if you have signs of an infection before, or while taking Venclexta, including: fever or chills, feeling weak or confused, cough, runny nose, sore throat; congestion on the chest; or pain or burning when passing urine. Some of the less serious side effects of Venclexta include diarrhoea; tummy pain; constipation, nausea (feeling sick); vomiting; reduced appetite; weight loss; mouth sores; looking pale; feeling tired; having little or no energy; shortness of breath when exercising; feeling dizzy; headache; low blood pressure; bleeding. Tell your doctor or pharmacist if you notice anything else that is making you feel unwell. Some medicines and Venclexta may interfere with each other, so tell your doctor if you are taking medicines containing any of the following: ketoconazole, posaconazole, voriconazole, itraconazole, fluconazole, clarithromycin, ciprofloxacin, erythromycin, ritonavir, diltiazem, verapamil, captopril, felodipine, dronedarone, amiodarone, quinidine, rifampicin, carvedilol, ciclosporin, quercetin, ranolazine, ticagrelor, azithromycin, nafcillin, carbamazepine, phenytoin, St John’s wort (Hypericum perforatum), bosentan, efavirenz, etravirine, modafinil, warfarin, digoxin, everolimus, or sirolimus. Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without prescription. Tell any other doctors, pharmacists, dentists, or surgeons treating you that you are taking Venclexta and remind them before you start any new medicines. If you have any questions about using Venclexta, including its risks and benefits, how much to use, how and when to use it, or storage conditions, ask your healthcare professional and refer to the Consumer Medicine Information (CMI) available from www.medsafe.govt.nz or free phone 0800 900 030. Ask your doctor if Venclexta is right for you. Use strictly as directed. If symptoms continue, or you have side effects, see your doctor, pharmacist, or healthcare professional. V7a.
©2026 AbbVie. All rights reserved. AbbVie® is a registered trademark of AbbVie Inc. VENCLEXTA® and its designs are registered trademark of AbbVie Manufacturing Management Unlimited Company. AbbVie Limited, PO Box 11437, Manners Street, Wellington 6142. TAPS BG5144. NZ-VEN-200006. ONO0212. April 2026.

